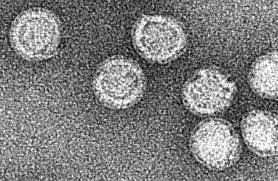
Tick-Borne Diseases – Prevention and Control
Many of our patients with cognitive decline are testing positive for tick-borne diseases including Lyme borreliosis, tick-borne encephalitis (TBE) and co-infections.
Here’s what you can do to prevent tick-bites and their associated diseases:
As the incidence of tick-borne illnesses is rising, it becomes increasingly important that we create awareness for our patients on how to prevent infection. In Europe, tick-borne diseases to be aware of include:
- Lyme borreliosis
- Tick-borne encephalitis (TBE)
- Tick-borne relapsing fever (TBRF)
- Crimean-Congo haemorrhagic fever (CCHF)
- Mediterranean spotted fever (MSF)
Tick-borne diseases are infectious diseases transmitted by the bites of infected ticks which can range from pinhead to pea size. Ticks climb up on plants and latch on to a passing host by using hooks on their legs.
The habitat of ticks vary from shady woodlands, clearings with grass, open fields and bushes (can vary depending on the tick species) and they are present in urban areas also. Although they are most active from spring to autumn, bites have been recorded all year round. Due to various factors, there are now more ticks in the UK as well as Europe.
People who engage in outdoor activities (e.g. hunting, fishing, hiking, camping, collecting mushrooms and berries, forestry and farming) are potentially at risk of infection by contact with infected ticks.
How to prevent tick bites
- Wear long-sleeved shirts and long trousers tucked into socks.
- Wear clothes with light colours to make it easier to spot ticks.
- Use tick repellent on clothes and skin.
- Avoid areas with ticks: high grasses, ferns etc.
It is important to inspect your body after being outdoors. Pay attention to the armpits, groin, legs, neck and head. If you do find a tick it is important to safely remove the tick with tick removal tools to ensure you get the head out, then clean the wound with antiseptic. Save the tick to send away for analysis.
Lyme borreliosis
This is currently the most prevalent tick-transmitted infection in temperate areas of Europe, North America and Asia. The infection can be asymptomatic for decades, making it difficult to diagnose. In less than 20% of cases there will be a bull’s eye rash that forms around the bite if one is infected. No laboratory tests are required in the diagnosis of a bull’s eye rash but if no rash appears, testing is still indicated. Antibodies to B. burgdorferi are usually detectable within 4-8 weeks of infection
Early treatment can prevent the risk of developing late stage complications. Even patients with late stage Lyme can benefit from antibiotics, although clinical recovery may be incomplete.
Written by Charmaine Shepherd
To find out more about the Bredesen Protocol and how it can help you, click the button below.
